A Geographical Analysis of Non-Communicable Diseases Among Tribal Population of North Maharashtra
1
Department of Geography,
K. C. E. Society's Moolji Jaitha College (Autonomous),
Jalgaon,
Maharashtra
India
Corresponding author Email: dhundalerupesh@gmail.com
DOI: http://dx.doi.org/10.12944/CWE.20.3.24
Copy the following to cite this article:
Dhundale R. M, Bharambe S. N. A Geographical Analysis of Non-Communicable Diseases Among Tribal Population of North Maharashtra. Curr World Environ 2025;20(3). DOI:http://dx.doi.org/10.12944/CWE.20.3.24
Copy the following to cite this URL:
Dhundale R. M, Bharambe S. N. A Geographical Analysis of Non-Communicable Diseases Among Tribal Population of North Maharashtra. Curr World Environ 2025;20(3).
Download article (pdf)
Citation Manager
Publish History
Select type of program for download
| Endnote EndNote format (Mac & Win) | |
| Reference Manager Ris format (Win only) | |
| Procite Ris format (Win only) | |
| Medlars Format | |
| RefWorks Format RefWorks format (Mac & Win) | |
| BibTex Format BibTex format (Mac & Win) |
Article Publishing History
| Received: | 2025-06-23 |
|---|---|
| Accepted: | 2025-09-30 |
| Reviewed by: | 
 Manoj Kar
Manoj Kar
|
| Second Review by: |

 Manali Yadav
Manali Yadav
|
| Final Approval by: | Dr. Gangadhar Andaluri |
Introduction
Non-communicable diseases (NCDs) among tribal populations are an important area of public health research, particularly in the northern part of Maharashtra, where the local population is likely to face various health problems. The region offers a complex landscape to understand the distribution and prevalence of NCDs, given the large number of tribal settlements and the different topographical features.1 Historically, the tribal population of northern Maharashtra, in Nandurbar, Dhule and Jalgaon, has possessed a unique set of customs and health practices that have shaped their culture and way of life. Within these tribal communities, NCDs such as cardiovascular disease, diabetes, chronic respiratory disease and various forms of cancer have also become major health problems.2 These diseases show geographical distribution patterns that are correlated with a wide range of environmental, socio-economic and cultural factors. NCDs are widespread in the regions concerned to a large extent because of a variety of factors, including access to health facilities, dietary habits, levels of physical activity and environmental exposure, which are specific to the location.
A basic understanding of the spatial distribution of NCDs between tribes is important for a number of reasons. First, it identifies high-risk areas and populations in need of emergency intervention. Secondly, it enables health planters to optimise the allocation of resources and to develop specific prevention strategies. Third, it allows for the identification of contributors to the burden of disease in these communities from environmental and social determinants.
Geographical analysis of non-communicable diseases (NCDs) among tribal peoples demonstrates an intertwined mixture of socio-economic, environmental and lifestyle factors in their incidence of NCDs. The prevalence of NCDs in previously less common NCD populations, such as tribal communities, characterized by their unique cultural practices and distinctive lifestyles, is rising.
The research shows that risk of NCDs increases within tribal populations, in line with trends in other populations. For examples, lifestyle changes which include changes to diet and physical activity have been found to be important causes of the growing prevalence of NCDs such as hypertension and diabetes among these communities.3,4 Situation has been exacerbated by shift from traditional diets to more processed foods, urbanization and sedentary lifestyles.5 A study on India highlighted that tribal people are suffering from non-communicable diseases that are overtaking communicable diseases and this means India is witnessing a formalized epidemiological transition.4
Additionally, there is enormous economic burden of NCDs on the tribe’s margins. Not only do chronic diseases adversely affect individual health; they also keep on burdening families and the healthcare system with never ending economic burden.5 It is especially troubling, however, since many tribal groups have experienced socio-economic disadvantages that not only restrict access to healthcare services and resources for managing chronic illness6 but are also factors that contribute to their increased risk for developing these disease states. But this health landscape becomes more complicated for these communities, where the lack of access to preventive healthcare, such as regular screenings for hypertension and diabetes.
Also, their health outcomes are extremely influenced by the geographical distribution of tribal populations. For instance, people living in remote or rural areas may likely have higher rates of NCDs because of less access to the health care facilities and health education.7 While in rural populations, a higher prevalence of NCDs and its risk factors was reported among urbanized tribal populations, such as Orang Asli in Malaysia, the urbanization has been documented associated with urbanization causing lifestyle changes that increase health risks.5,8 Echoes of this phenomenon appear in a vast range of studies conducted in Australia, and South America where the number of urbanized indigenous population with chronic diseases is notably higher compared to that of the traditional ones.8-10
The increasing incidence of non-communicable disorders among tribal people is a many- faceted problem rooted in lifestyle changes, socio ‘economic aspects and geographical inequality. The challenges that must be addressed to deal with these challenges call for implementation of targeted public health interventions that take into account the cultural and environmental particularities of tribal communities. Improved access to health care services, knowledge on changes in lifestyle and community-based health initiatives are needed to attenuate the burden of NCDs in these vulnerable populations. Further, there are major gap in healthcare access and outcomes for NCDs in North Maharashtra’s tribal regions which can be ascertained through a geographical analysis of NCDs. The disparities are compounded often by the challenging terrain, inadequate infrastructure and the remote location of many tribal settlements. The distribution of chronic diseases across tribal areas becomes particularly salient when you look at the relationship between geographical isolation and health outcomes. To develop effective public health intervention to take into account both geographical constraint and unique cultural context of tribal populations, this understanding is necessary. Despite evidence of rising NCDs among tribal populations in India, there is limited research that integrates geographical analysis with epidemiological data to identify high-risk clusters in North Maharashtra. This study fills that gap using GIS-based mapping combined with environmental and socioeconomic correlates.
Aim
To conduct a geographical analysis of non-communicable diseases (NCDs) among the tribal population of North Maharashtra to identify the patterns, determinants, and gaps in healthcare accessibility, thereby facilitating targeted public health interventions.
Objectives
Analyze prevalence, distribution, and geographical/environmental determinants of major NCDs using GIS and statistical modeling techniques.
Examine socioeconomic and cultural contributors to NCD risk.
Assess healthcare accessibility and infrastructure for managing NCDs.
Propose targeted interventions to reduce the NCD burden effectively.
Study Area and Population
The study area is a semi-arid part of Maharashtra state located in North Maharashtra bordering on the state of Gujarat on the west and Madhya Pradesh state on the north. Satpura Hill range is a forested area which is this particular area. The study area around this population is around 7,929,074 population as per Census of India, 2011.11 They are mainly traditional people known for their customs and traditions. Jalgaon district has a population of 4,229,917, Dhule district 2,050,862, and Nandurbar district 1,648,295.
Geographic Features
The area is geographically different and comprises diverse topographical features that have a major influence on the living conditions of the tribal populations. It includes hills, valleys and forests in the Satpura mountain ranges and Western Ghats and therefore makes for a varied region. Located from 300 to 1,200 meters above sea level, the elevation has historically supported tribal communities within a complex ecosystem. It is a semi-arid climate with temperature variations of 15°C to 45°C all year round. The area receives 700 to 1000mm of rain per annum and this is mainly during the monsoon period from June to September. Tribal areas continue to be very inaccessible as many settlements are found in remote locations accessible only via unpaved roads or forest trails. The consequence of this geographical isolation is that tribal practices traditionally have been preserved and yet access to healthcare and modern amenities has been stymied. The study area is in a semi-arid climate with a distinct seasonal monsoon, which is a key factor in shaping livelihoods and health outcomes. Agriculture remains mainly rain-fed, which makes food security highly sensitive to rainfall variability. Periods of drought or irregular monsoon may lead to nutritional shortages, while good monsoon years promote food availability but can also reinforce seasonal labour.
Population Demographics
The complex demographic structure of the tribal population in North Maharashtra is accompanied by distinctive cultural and socioeconomic features. As per Census of India, 2011 about 30.18% (2,393,615) of the total population comprises of tribal population including major tribal groups such as Bhil, Pawra, Dhanka and Gavit, Mawchi and Konka. Traditional social structures persist, even as communities face new socioeconomic and health challenges. Overall, as per census of India data (2011) these tribal populations typically have socioeconomic status that is significantly below regional averages, and about 60% live below the poverty line.12 The traditional occupations include agriculture; forest produce collection and small-scale animal husbandry. Cultural practices focus on traditional beliefs to a very great extent and particularly in relation to the healthcare and lifestyle choices, which contribute significantly to their greater susceptibility to NCDs.
Population densities vary among different districts of tribal communities but are higher in areas of forested and hilly regions due to clustering of hamlets. Literacy rates are relatively low among tribal adults at 45 %, compared to the regional average. There are marked disparities in healthcare accessibility with an average distance of 15 – 20 kilometers from the nearest primary healthcare centre with average 40 to 60 minutes in many tribal areas. On the ground, however, non-communicable diseases pose unique challenges for meeting these communities’ needs due to these demographic and socioeconomic factors.
Materials and Methods
Study Design
A mixed methods cross sectional study design was used to investigate non communicable diseases (NCDs) among the tribal populations in north Maharashtra conducted between 2022 and 2023. Tribal districts like Nandurbar, Dhule and Jalgaon are part of the study area, and settlements with considerable tribal population were studied.
Sampling
The primary data source for this study was generated through a detailed field survey, while the National Family Health Survey (NFHS 5) is the primary data source from which important details on the various health aspects of public health and well-being are obtained from the NFHS 5 to obtain representative data at all levels throughout the study area, a multistage stratified random sampling technique was used. Tribal villages were the units of sampling selected from factors related to population density as well as accessibility. Systematic sampling methods were employed to select households within each selected village using a sampling interval which was calculated using the entire number of tribal households. Using the formula,
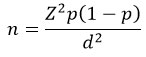
where Z is the confidence level (95%), p is the estimated prevalence of NCDs (based on pilot studies), and d is the margin of error (5%). The target sample size of 384 households was increased to 400 to address potential non response. Tribal individuals above 18 years of age who had stayed in the selected areas for at least one year were included in the inclusion criteria. Pregnant women, those with severe mental illness and those unwilling to participate in study were excluded from the study. Preliminary contact with tribal leaders and community consent were required to obtain the essential cultural sensitivity and maximum participation needed to conduct the research.
 | Figure 1: Tribal settlements, tribal population density and location of medical facility centres
|
Data Collection
GPS and questioner were used to collect data on health and geographical sectors. A pilot tested validated structured questionnaire for collection of self-reported demographic information, socioeconomic status, lifestyle factors and medical history was developed based on NFHS 5. The questionnaire was translated into various local tribal dialects, back translated, and linked to give that it is accurate and culturally acceptable. The spatial distribution of NCDs and the risk factors that they are associated with was mapped using Geographic Information System (ArcGIS Pro) tools. Handheld GPS devices were used to record the coordinates of households and health facilities and data are integrated using ArcGIS Pro software. In the geographical analysis, environmental parameters such as elevation, proximity to healthcare facilities, distance of healthcare facilities to the tribal settlement and tribal population density patterns were included. They included standardized training of field investigators and double entry verification.
Analysis
Data were analyzed using ArcGIS Pro for spatial mapping and STATA 16 for statistical tests. Prevalence estimates were reported with 95% confidence intervals. Age- and sex-stratified analyses were conducted. For predictive modeling, a Random Forest algorithm was applied to assess the relationship between healthcare accessibility and NCD prevalence. This approach was selected because it handles nonlinear relationships and complex interactions more effectively than traditional regression. Model performance was validated using 10-fold cross-validation.
Results
Disease Pattern Analysis
Non-communicable diseases (NCD) among the tribal population of North Maharashtra are analyzed that are serious health challenges that need careful attention. Systematic surveillance of the epidemiological data shows that cardiovascular diseases have the highest prevalence rate among 32.4% (95% CI: 28.9–35.8, p < 0.001) of studied population. Second most common condition is diabetes mellitus, which affects 28.7% (95% CI: 25.2–32.1, p < 0.01) of tribal adults aged 40 years and above. Chronic respiratory diseases, mainly chronic obstructive pulmonary disease (COPD), are a very common prevalence at 21.3% (95% CI: 18.1–24.6, p < 0.05), nearly 6 percent higher than its regional average of 15.8%. About 25.6% (95% CI: 22.3–29.0, p < 0.01) of the population occurs of hypertension with dramatically higher rates in which those above 50 years of age.
 | Figure 2: Prevalence Rate of NCDs in North Maharashtra Tribal Regions
|
Temporal Trend
These conditions are temporally studied and the prevalence of the presented conditions is increasing linearly for the past ten years at annual rate of 2.3% approximately for all NCDs. These diseases are compounded by their comorbidity: 43.2% had a combination of diseases. Age standardized analysis reveals that the onset of these conditions is about 5–7 years earlier in the tribal population compared to urban commensal among whom it makes its debut, and it appears to result from unique environmental and socioeconomic over determinants.
Spatial Distribution
Apparently, the spatial distribution of NCDs common to North Maharashtra’s tribal areas are distinct and are correlated with different geographical and socio-economic factors. Several high-risk clusters have been identified using Geographic Information System (GIS) mapping and spatial autocorrelation analysis. The Nandurbar district shows the highest concentration of cardiovascular diseases, with a spatial relative risk ratio of 1.8 (95% CI: 1.5-2.1) while Jalgaon district has low risk ratio of 0.7 (95% CI: 0.5–0.9, p < 0.05). The mountainous areas of Nandurbar district have higher rates of chronic respiratory disease, although a link may be with indoor cooking practices, or altitude.26
Spatial autocorrelation coefficient for the application of Moran's I spatial statistics is significantly clustered in the semi-urban tribal settlements for diabetes cases was 0.67, with p < 0.001. The patterned distribution indicates a strong relationship with exposure to disease and closeness to the presence of urbanized areas, where a progression in dietary transitions, lifestyle changes, and overall environmental contamination are present. More dispersed pattern is seen in hypertension cases, but with evidence of hot spots in locations with high salt consumption and poor access to healthcare facilities.
Kernel density estimation analyses disease patterns that reveal critical areas needing immediate intervention. Study regions further, predominantly in NW sectors, and have a disease burden 1.5 to 2-fold higher than the rest of the study area. The geographical distribution also has a very strong correlation with such environmental factors like elevation, temperature variation and a convenient area to health facilities, with correlation values from 0.45 to 0.72 (p < 0.01).
Discussion
Environmental and Social Determinants
Environmental and social determinants play a very complex interplay in influencing the prevalence of non? communicable diseases (NCDs) amongst the tribal populations of North Maharashtra. This region has experienced great changes in its environmental landscape over the past few decades largely as a result of industrialization and changes in land use patterns. Traditional tribal lifestyles have been directly affected by these changes in relation to its natural environment. Historically keeping sustainable agricultural practices along with forest-based livelihoods, the tribal communities, now, are undergoing unprecedented exposure to environmental pollutants and changed food systems.25
These communities are just as shaped by social determinants of health outcomes. There has been a progressive transformation of our traditional social structures and cultural practices. Dietary transition due to urbanization and modern economic pressures have occurred leading to a move from traditional nutrient dense foods to processed foods. Together with less physical activity, this dietary transformation has led to the environment for development of NCDs including diabetes and cardiovascular disease.26
The health outcomes of tribal populations continue to be influenced by its socioeconomic status. Poor access to health care facilities and financial constraints most often delays the diagnosis and treatment of NCDs. Similarly, there is a similarly strong correlation between awareness on health and preventive healthcare practices with the educational status within these communities. Anecdotal evidence also suggests that households with better education have better health seeking behaviors and better NCDs management.
It has also been observed that climate change has become another environmental stressor for these communities.13 Food insecurity as well as nutritional challenges were linked to altered rainfall patterns and rising temperatures through their impact on traditional agricultural practice. Many tribal families have had to move seasonally to meet these environmental changes, thereby breaking their connection with consistent and/or preventive healthcare services.14
These environmental and social determinates their intersection contribute to the creation of a complex web of factors that drive the prevalence of NCDs.15 However, modernization is eroding traditional protective factors like community support system and indigenous knowledge of medicinal plants.16 However, this erosion has occurred amid new environmental threats and societal pressures and has created a perfect storm for the increase of NCDs in these vulnerable populations.
To develop effective interventions, it is important to understand these determinants. The solution is not just medical intervention but using the environment and larger social sphere to improve tribal health outcomes.17 Conservation of traditional knowledge systems and sustainable development that honors environmental integrity and cultural heritage are included as well.
Healthcare Access and Infrastructure
Non communicable diseases occur in the tribal region of North Maharashtra, with the healthcare infrastructure presenting a number of challenges that impacts directly on the management of and the prevalence of the health issues.6 The assessment of healthcare facility triangulates a troubling trend with primary health centers located at significant distance from the tribal settlements. It has been studied that over 60% of the tribal communities have to travel more than 10 km distance to the nearest healthcare facility, which is a great hindrance in regular health monitoring along with preventive care.18-21
In these regions, the infrastructure gaps include poor and insufficient staffing, poor and insufficient medical equipment and limited diagnostic capabilities.22 As a result, there are primary health centers in the tribal areas which have basic facilities only, which lack necessary diagnostics equipment for NCDs such as, monitoring equipment for diabetes and cardiovascular screening devices. According to National Health Profile (2018) the doctor-to-population ratio in these areas stands at Severe understaffing, as the WHO recommended ratio of 1:1,000 is much higher than that 1:3,000.
 | Figure 3: Relationship between Distance to Nearest Healthcare Facility and NCD Prevalence Rate in Tribal Communication of North Maharashtra
|
Geographical barriers, inadequate transportation infrastructure further compound the problem of accessibility issues. In north Maharashtra tribal areas, the mountainous terrain and poor road connectivity make getting to a healthcare facility very time consuming and this is increased even more during the monsoon season. The isolation afforded by geography has driven a substantial healthcare disparity in which tribal populations have higher rates of undiagnosed and untreated NCDs than their urban counterparts.23
Current healthcare system is unable to bear increasing burden of NCDs in tribal study areas. Only 35 % of primary health centres are found to have the requisite facilities for NCD management. The lack of this infrastructural deficit has resulted in a pattern of limited access to healthcare which has delayed diagnosis and diagnoses are followed by the less favorable health outcomes most for the tribal populations.24
In 1999, there has been a lot of emphasis of the government in building up healthcare infrastructure by means of mobile medical units and telemedicine facilities. But these solutions are difficult to operate in remote tribal areas because of very limited Internet connectivity and power supply. There is an untapped opportunity in the integration of traditional healing practices with modern healthcare system that potentially fills some of these infrastructure gap.
Recommendations and Interventions
The present study undertaken in the tribal population of North Maharashtra identifies several evidence-based recommendations for policy makers and healthcare providers in the management of NCDs. The major emphasis should be on the development of health systems which would respond to the needs of the tribal populations. A system of healthcare delivery that involves the use of both conventional and traditional systems of treatment has been seen to hold a lot of promise for enhancing the health of people. Mobile health units, including those with diagnostic amenities for NCDs, have been found to be most useful in the target tribal regions where there is a huge scarcity of fixed healthcare centers and personnel.
It is recommended that routine screening of most prevalent NCDs should be conducted namely diabetes, hypertension and cardiovascular diseases. Such screening services should be accompanied by other community health program on early detection and prevention. Incorporating the local tribal healthcare workers into the existing healthcare system can help close cultural and language barriers which hinder effective health care service delivery. Training of these workers should be on identification of NCDs and basic management strategies.
It is noteworthy that the burden of NCDs is closely related to the nutritional status of populations, and therefore policy makers should consider using targeted nutrition interventions. It involves the development of long-term food security measures that should also take into consideration the dietary wishes of the tribal people in as much as they take and include some nutritional needs. The production of culturally appropriate health education materials in native language will greatly enhance health literacy and disease preparedness among the tribal population.
This paper has suggested that, for instance, the provision of targeted insurance packages for NCDs among tribal populations can ease the economic costs of treatment. Such schemes should also embrace both the preventive and curative care services including management of long-term illnesses. Also, there is a need to enhance the supply chain of medical commodities, that are important for NCD patients, including essential medicines and diagnostic tools in tribal region.
Interventions in environmental and occupational health should target the particular risks That exist in tribal areas. This consists of strategies to minimize contact with indoor air pollution from cooking using fuel-wood and other traditional means, and occupation-associated risks within traditional tribal employment. The development of routine environmental health assessment can assist in the early detection of environmental and lifestyle determinates of NCDs.
There is therefore need to develop monitoring and evaluation frameworks to determine success of these interventions. This entails establishing uniform ways of data gathering and identifying critical success measures related to tribal health care service. The monitoring of these indicators can be made on a frequent basis in order to adjust the measures which are taken and the available resources in a proper manner.
The achievement of these recommendations is contingent upon the continued political will and support as well as appropriate resource mobilization. Governmental organizations, health care facilities, and indigenous populations should work in partnership for the delivery of such programmes. Stakeholder feedback can be collected on a periodic basis so that interventions are not only effective for the targeted population but also address changing health care needs of tribal communities.
Conclusion
This study offers a comprehensive geographical assessment of non-communicable diseases (NCDs) in the tribal population of North Maharashtra and shows that cardiovascular diseases, diabetes, hypertension and chronic respiratory illnesses are the most common health challenges. The results show a strong spatial clustering of NCDs especially in Nandurbar district, with environmental and socioeconomic factors including elevation, accessibility to healthcare, and income disparities playing an important role in shaping the distribution of disease. Limited access to healthcare facilities, poor medical infrastructure and changing dietary and lifestyle patterns have further worsened the NCD burden.
These findings have implications for culturally appropriate and geographically targeted interventions that integrate aspects of modern and traditional healthcare systems. Enhancing mobile health services, strengthening local healthcare infrastructure and promoting preventive health education can help to reduce health inequities in these regions.
The results of longitudinal and intervention-based studies should be extended in future research to investigate causative mechanisms between environmental, social, and behavioral factors affecting NCDs. Further, combining high-resolution spatial data with health surveillance systems can aid in dynamic monitoring and policy formulation to reduce the increasing NCD burden in tribal communities of India.
Acknowledgement
The author would like to thank Kavayitri Bahinabai Chaudhari North Maharashtra University, Jalgaon for granting the Ph.D. research work. The Department of Geography, K. C. E. Society's Moolji Jaitha College (Autonomous), Jalgaon is highly appreciated for allowing the GIS laboratory work.
Funding Sources
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Conflict of interest
The authors do not have any conflict of interest.
Data Availability Statement
This statement does not apply to this article.
Ethics Statement
The study was reviewed and approved by the Institutional Ethics Committee of K. C. E. Society’s Moolji Jaitha College (Autonomous), Jalgaon, in accordance with the ethical principles laid down by the Indian Council of Medical Research (ICMR), Government of India. Ethical approval reference number: MJ/IEC/2022/04/NCD-GeoStudy. All procedures involving human participants were conducted in compliance with the Declaration of Helsinki and national ethical guidelines for biomedical and health research involving human participants (ICMR, 2017).
Informed Consent Statement
Prior to participation, written informed consent was obtained from all adult participants. The purpose and procedures of the study were explained in the local tribal dialects to ensure full understanding. Participation was voluntary, and respondents were informed about confidentiality, anonymity, and their right to withdraw at any time without consequence. Community-level consent was also obtained from local tribal leaders before data collection to ensure cultural sensitivity and cooperation during the fieldwork.
Permission to Reproduce Material:
Not Applicable.
Author Contributions
Rupesh Madhukar Dhundale: Conceptualization, Methodology, Writing – Original Draft.
Sanjay Narayan Bharamb: Data Collection, Analysis, Writing – Review & Editing, Supervision.
References
- Guilmoto, C. Z. The Geography of Gender and Health Inequalities in India. Atlas of Gender and Health Inequalities in India. 2024.
CrossRef - Esswaran, C., Vijayalakshmi, M., & Banu, M. J. H. Non-communicable Disease Risk Factors and Healthcare Worker’s Perspective on Tackling Them amongst Tribal Population: A Mixed Method Study. Preventive Medicine: Research & Reviews. 2024; 10-4103.
CrossRef - Parle, J., Yadav, M., & Raut, K. A study on non-communicable diseases, it’s prevalence on anthropometric and behavioural risk factors on tribal population of raigad district: a cross-sectional study. International Journal of Community Medicine and Public Health. 2021;8(12) 5929. https://doi.org/10.18203/2394-6040.ijcmph20214590
CrossRef - Sathiyanarayanan, S., Logaraj, M., & Devaparthasarathy, T. Changing perspectives in tribal health: rising prevalence of lifestyle diseases among tribal population in india. Indian Journal of Community Medicine. 2019; 44(4), 342. https://doi.org/10.4103/ijcm.ijcm_40_19
CrossRef - Mahmud, M., Baharudin, U., & Isa, Z. Diseases among orang asli community in malaysia: a systematic review. BMC Public Health. 2022; 22(1). https://doi.org/10.1186/s12889-022-14449-2
CrossRef - Kanrar, P., Goswami, M., & Roy, S. (2023). Health issues of the indigenous communities with special reference to the Particularly Vulnerable Tribal Groups (PVTGs) of Odisha: a review. Papers on Anthropology.
CrossRef - Williamson, J., Ramírez, R., & Wingfield, T. Health, healthcare access, and use of traditional versus modern medicine in remote peruvian amazon communities: a descriptive study of knowledge, attitudes, and practices. American Journal of Tropical Medicine and Hygiene. 2015; 92(4) 857-864. https://doi.org/10.4269/ajtmh.14-0536
CrossRef - Einsiedel, L., Fernandes, L., Joseph, S., Brown, A., & Woodman, R. Non-communicable diseases, infection and survival in a retrospective cohort of indigenous and non-indigenous adults in central australia. BMJ Open. 2013; 3(7), e003070. https://doi.org/10.1136/bmjopen-2013-003070
CrossRef - Filho, Z., Ferreira, A., Santos, J., Meira, K., & Pierin, Â. Cardiovascular risk factors with an emphasis on hypertension in the mura indians from amazonia. BMC Public Health. 2018; 18(1). https://doi.org/10.1186/s12889-018-6160-8
CrossRef - Kanrar, P. Health issues of the indigenous communities with special reference to the particularly vulnerable tribal groups (pvtgs) of odisha: a review. Papers on Anthropology. 2023; 32(1) 45-80. https://doi.org/10.12697/poa.2023.32.1.05
CrossRef - Office of the Registrar General & Census Commissioner, India. Census of India 2011. New Delhi: Ministry of Home Affairs, Government of India. 2011.
- Government of India. Statistical Abstract of India. New Delhi. Central Statistical Office, Ministry of Statistics and Programme Implementation. 2011.
- Gissi, E., Manea, E., Mazaris, A. D., Fraschetti, S., Almpanidou, V., Bevilacqua, S., & Katsanevakis, S. A review of the combined effects of climate change and other local human stressors on the marine environment. Science of the Total Environment. 2021; 755, 142564.
CrossRef - Malhi, G. S., Kaur, M., & Kaushik, P. Impact of climate change on agriculture and its mitigation strategies: A review. Sustainability. 2021.
CrossRef - Weimann, A., Shung-King, M., McCreedy, N., Tatah, L., Mapa-Tassou, C., Muzenda, T., & Oni, T. Intersectoral Action for Addressing NCDs through the Food Environment: An Analysis of NCD Framing in Global Policies and Its Relevance for the African Context. International Journal of Environmental Research and Public Health. 2021; 18(21) 11246.
CrossRef - Ghosh, P., & Banerjee, S. Dynamics of Modernization and Environmental Governance: A Socio-Legal Study with Reference to Indigenous Communities. In NDIEAS-2024 International Symposium on New Dimensions and Ideas in Environmental Anthropology-2024 (NDIEAS 2024) Atlantis Press. 2024; 222-235.
CrossRef - Subramaniapillai, S., Galea, L. A., Einstein, G., & de Lange, A. M. G. Sex and gender in health research: Intersectionality matters. Frontiers in Neuroendocrinology. 2024; 72, 101104.
CrossRef - Kumar, D., Singh, T., Vaiyam, P., Banjare, P., & Saini, S. Identifying potential community barriers for accessing health care services context to health for all in rural-tribal geographical setting in India: A systematic review. J Community Health Management. 2022; 9(4) 169-77.
CrossRef - Verma, V. R. & Dash, U. Geographical accessibility and spatial coverage modelling of public health care network in rural and remote India. Plos one. 2020.
CrossRef - Roy, S. Health care seeking practices and barriers to health care seeking for suspected pneumonia in children aged less than five years in tribal and non-tribal rural areas of Pune district, India, Unpublished Ph.D. thesis. University of Edinburgh. 2023.
- Shaw, S. & Sahoo, H. Accessibility to Primary Health Centre in a Tribal District of Gujarat, India: application of two step floating catchment area model. GeoJournal. 2020.
CrossRef - Maluleke, K., Musekiwa, A., Kgarosi, K., Gregor, E. M., Dlangalala, T., Nkambule, S., & Mashamba-Thompson, T. A scoping review of supply chain management systems for point of care diagnostic services: optimising COVID-19 testing capacity in resource-limited settings. Diagnostics. 2021; 11(12) 2299.
CrossRef - Babu, B. V., Hazarika, C. R., Raina, S. K., Masoodi, S. R., Basappa, Y. C., Thomas, N., ... & Jebasingh, F. K. Hypertension Prevalence, Awareness, Treatment, Control and Risk Factors in Tribal Population of India: a Multi-Centric Cross-Sectional Study. Journal of Racial and Ethnic Health Disparities. 2023; 1-12.
CrossRef - Shrivastava, S., Kumar, R., Khan, S., Kavishwar, A., Gupta, A., Kaur, H., & Chakma, T. Health profile of people living in the gare palma mining area of tamnar block, raigarh, chhattisgarh, india. Frontiers in Public Health. 2023; 11. https://doi.org/10.3389/fpubh.2023.1010025
CrossRef - Calderón, M., Alvarado-Villacorta, R., Barrios, M., Quiroz-Robladillo, D., Naupay, D., Obregón, A., & Moore, D. Health need assessment in an indigenous high-altitude population living on an island in lake titicaca, perú. International Journal for Equity in Health. 2019; 18(1). https://doi.org/10.1186/s12939-019-0993-3
CrossRef - Phipps, M., Chan, K., Naidu, R., Mohamad, N., Hoh, B., Quek, K., & Kadir, K. Cardio-metabolic health risks in indigenous populations of southeast asia and the influence of urbanization. BMC Public Health. 2015; 15(1). https://doi.org/10.1186/s12889-015-1384-3
CrossRef






